科研进展
【文献导读】NEJM:新发卒中伴房颤的抗凝治疗:早期还是晚期应用?
Early versus Later Anticoagulation for Stroke with Atrial Fibrillation.
新发卒中伴房颤的抗凝治疗:
早期还是晚期应用?
文章来源:10.1056/NEJMoa2303048
编译:刘海雁,IE-learning翻译团队
Background
The effect of early as compared with later initiation of direct oral anticoagulants (DOACs) in persons with atrial fibrillation who have had an acute ischemic stroke is unclear.
背景
急性缺血性卒中房颤患者早期和晚期直接口服抗凝剂(DOAC)的效果差异尚不清楚。
Methods
We performed an investigator-initiated, open-label trial at 103 sites in 15 countries. Participants were randomly assigned in a 1:1 ratio to early anticoagulation (within 48 hours after a minor or moderate stroke or on day 6 or 7 after a major stroke) or later anticoagulation (day 3 or 4 after a minor stroke, day 6 or 7 after a moderate stroke, or day 12, 13, or 14 after a major stroke). Assessors were unaware of the trial-group assignments. The primary outcome was a composite of recurrent ischemic stroke, systemic embolism, major extracranial bleeding, symptomatic intracranial hemorrhage, or vascular death within 30 days after randomization. Secondary outcomes included the components of the composite primary outcome at 30 and 90 days.
方法
我们在15个国家的103个研究中心进行了一项研究者发起的开放标签试验。受试者以1:1的比例随机分配至早期抗凝治疗组(轻度或中度卒中后48小时内,或重度卒中后第6或7天)或晚期抗凝治疗组(轻度卒中后第3或4天,中度卒中后第6或7天,或重度卒中后第12、13或14天)。评估者不知道试验组分配。主要结局是随机分组后30天内复发性缺血性卒中、全身性栓塞、颅外大出血、症状性颅内出血或血管性死亡的复合终点。次要结局包括30天和90天时复合主要结局的组成部分。
Results
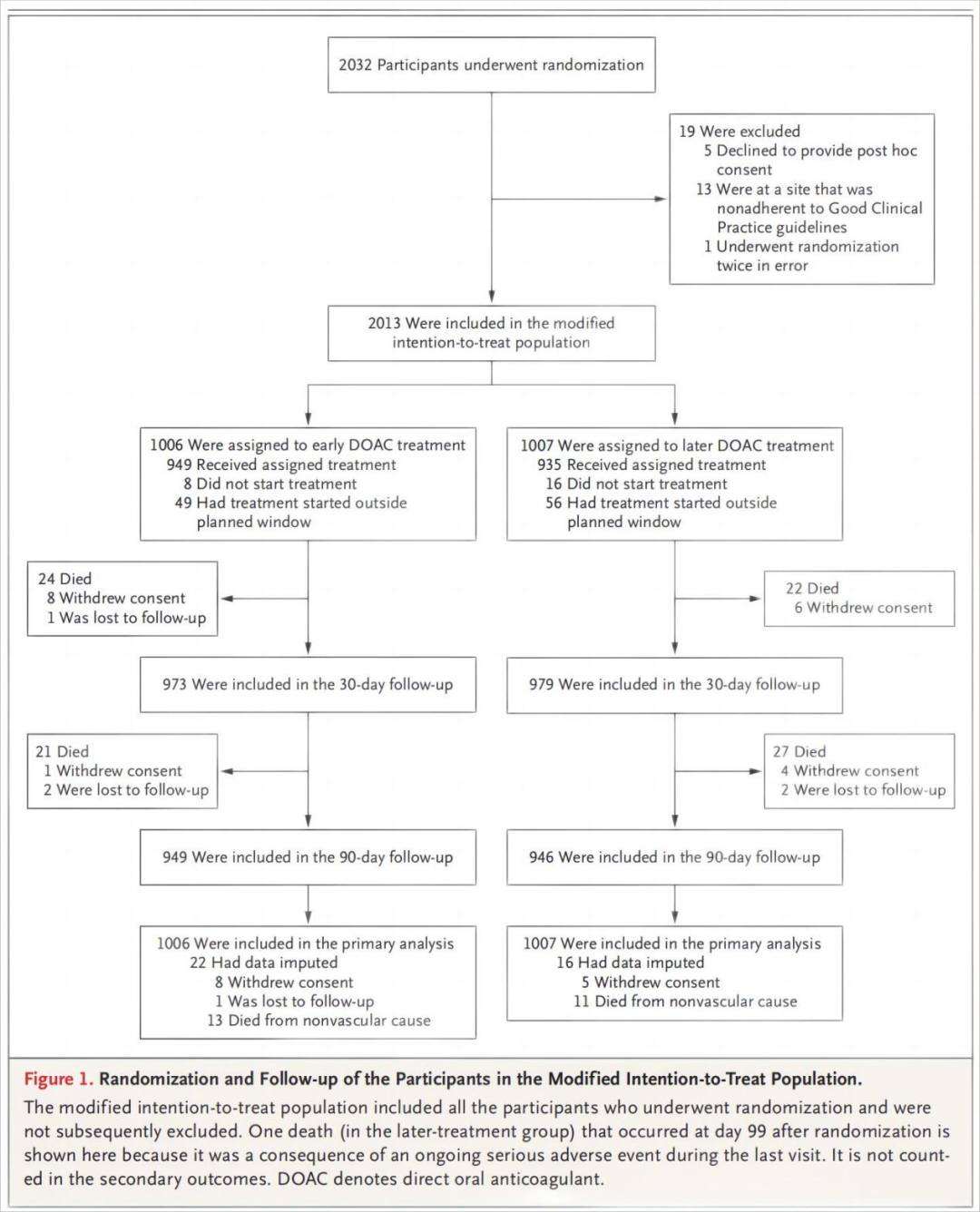
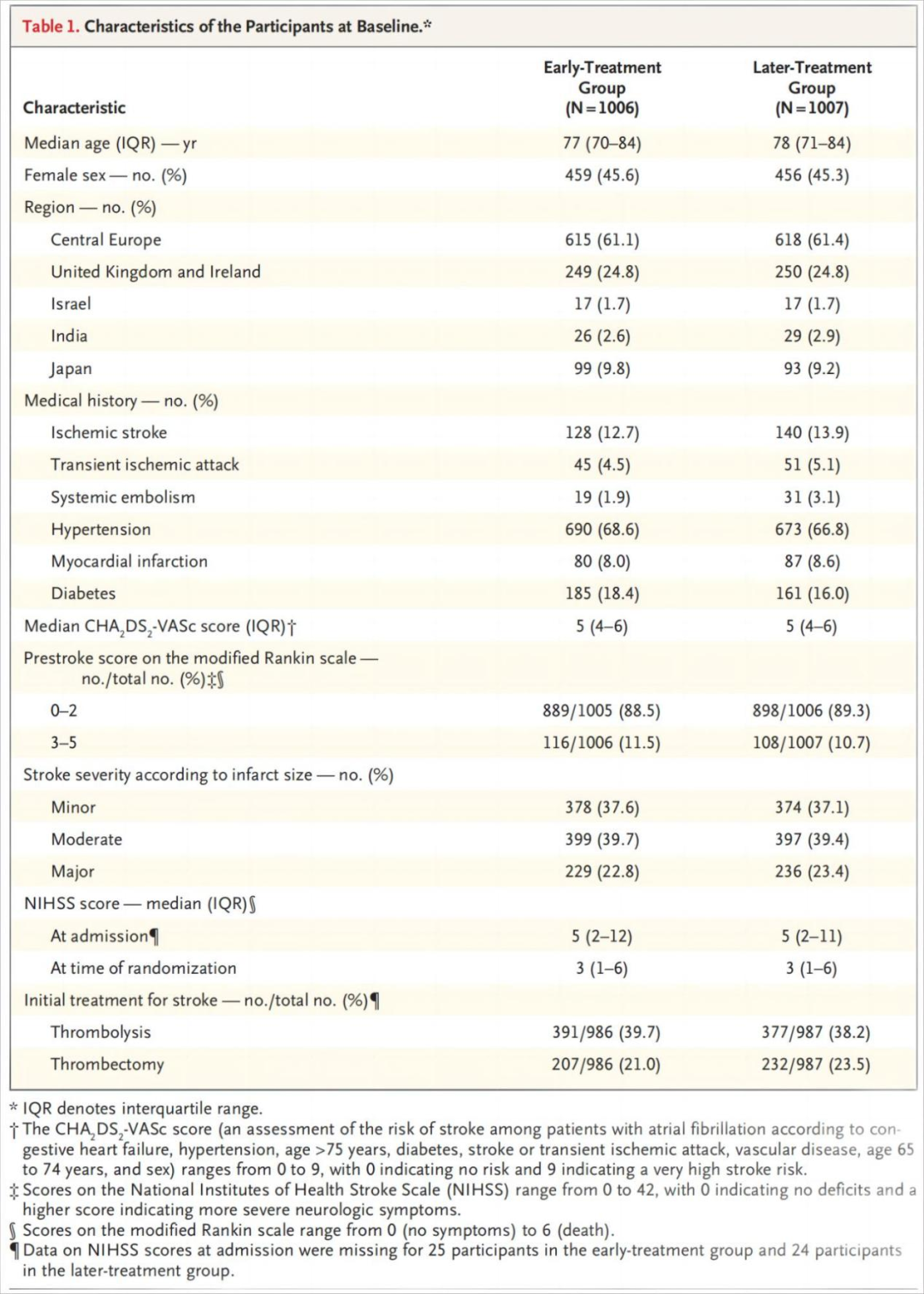
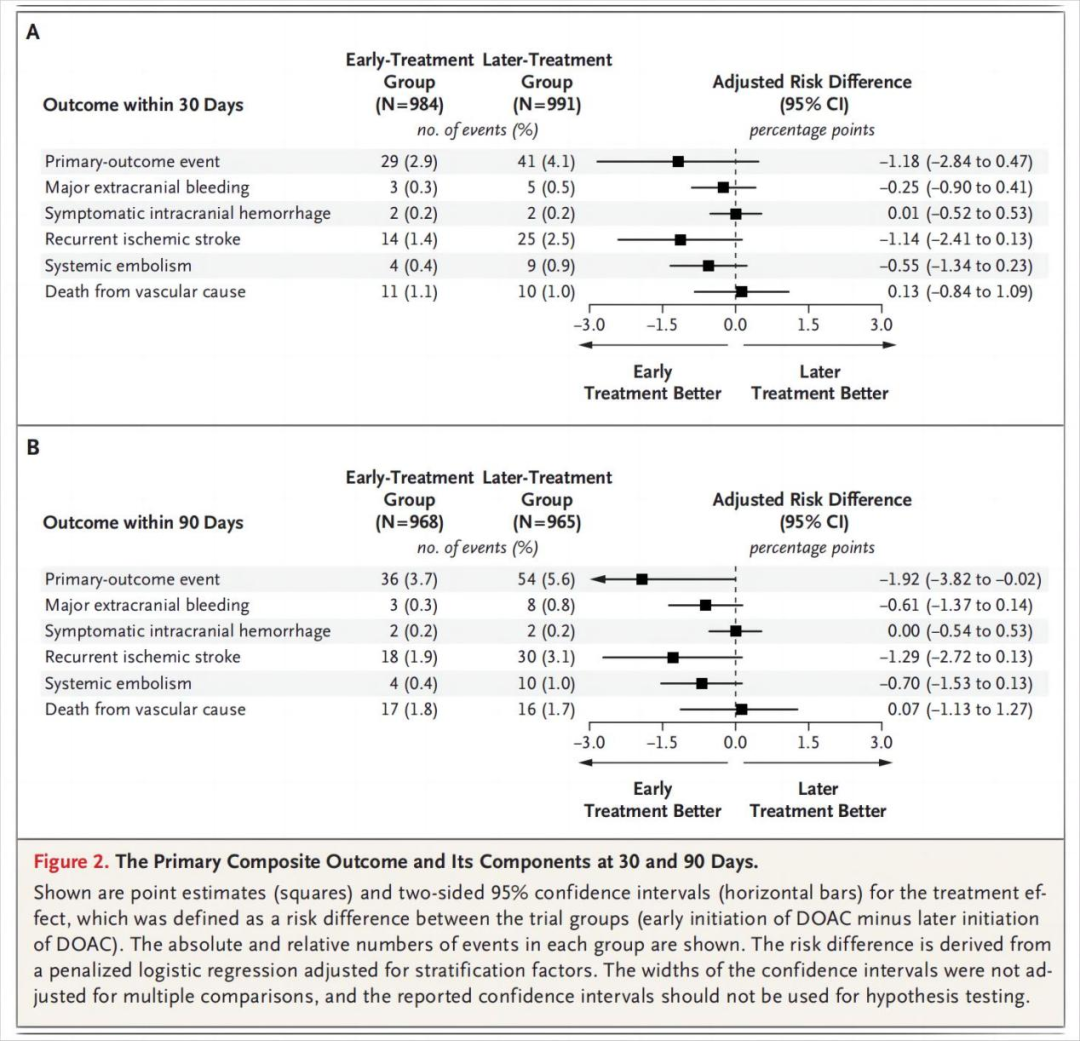
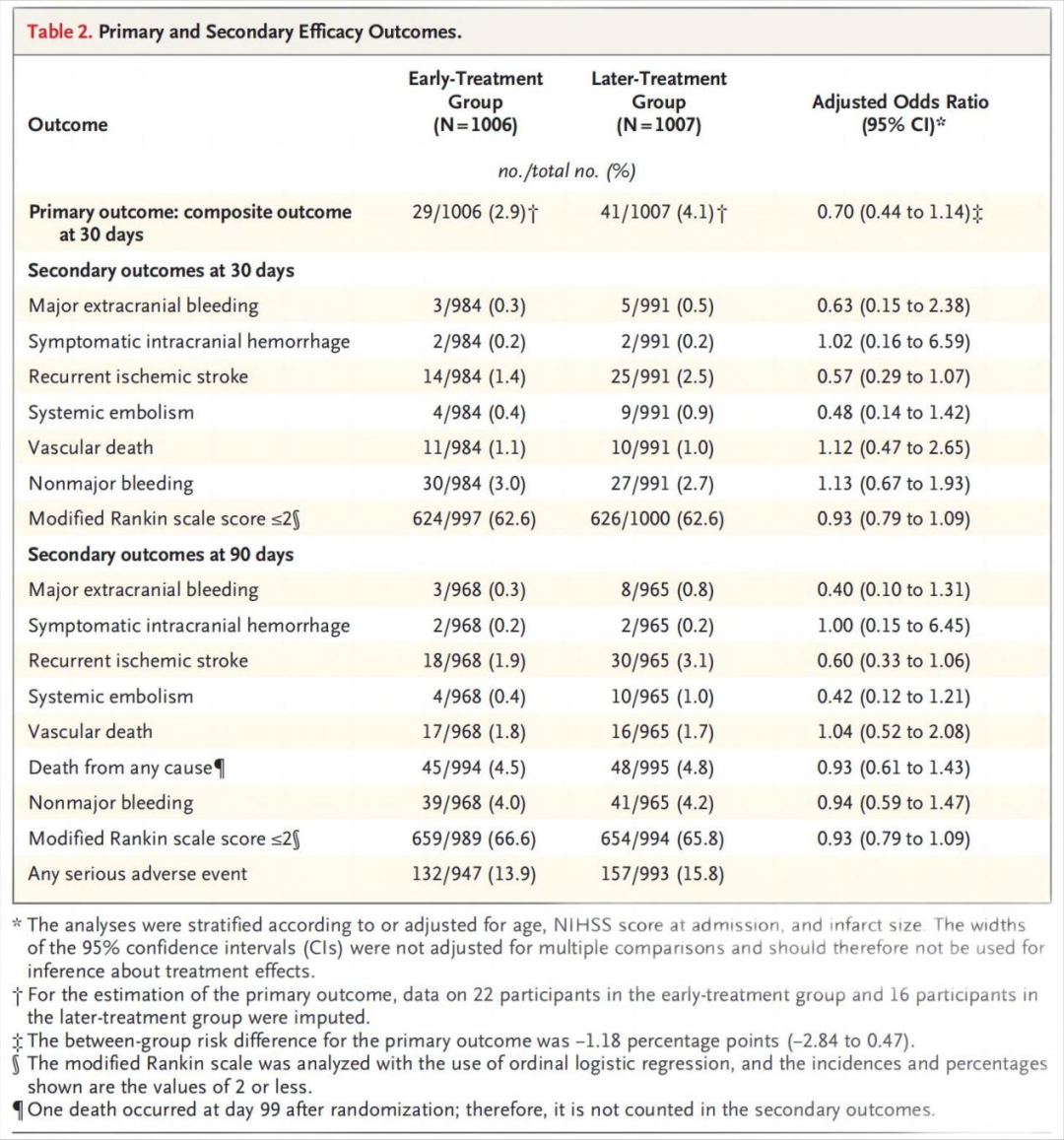
Of 2013 participants (37% with minor stroke, 40% with moderate stroke, and 23% with major stroke), 1006 were assigned to early anticoagulation and 1007 to later anticoagulation. A primary-outcome event occurred in 29 participants (2.9%) in the early-treatment group and 41 participants (4.1%) in the later-treatment group (risk difference, −1.18 percentage points; 95% confidence interval [CI], −2.84 to 0.47) by 30 days. Recurrent ischemic stroke occurred in 14 participants (1.4%) in the early-treatment group and 25 participants (2.5%) in the later-treatment group (odds ratio, 0.57; 95% CI, 0.29 to 1.07) by 30 days and in 18 participants (1.9%) and 30 participants (3.1%), respectively, by 90 days (odds ratio, 0.60; 95% CI, 0.33 to 1.06). Symptomatic intracranial hemorrhage occurred in 2 participants (0.2%) in both groups by 30 days.
在2013例受试者中(37%轻度卒中,40%中度卒中,23%重度卒中),1006例被分配接受早期抗凝治疗,1007例被分配接受晚期抗凝治疗。早期治疗组有29名参与者(2.9%)发生主要结局事件,晚期治疗组有41名参与者(4.1%)发生主要结局事件(风险差异,-1.18个百分点; 95%置信区间[CI],-2.84至0.47)。早期治疗组有14名参与者(1.4%)和晚期治疗组有25名参与者(2.5%)发生了复发性缺血性卒中(比值比,0.57; 95%CI,0.29 - 1.07),90天时分别有18例(1.9%)和30例(3.1%)受试者(优势比,0.60; 95%CI,0.33至1.06)。30天时,两组中均有2例受试者(0.2%)发生症状性颅内出血。
Conclusions:
In this trial, the incidence of recurrent ischemic stroke, systemic embolism, major extracranial bleeding, symptomatic intracranial hemorrhage, or vascular death at 30 days was estimated to range from 2.8 percentage points lower to 0.5 percentage points higher (based on the 95% confidence interval) with early than with later use of DOACs. (Funded by the Swiss National Science Foundation and others; ELAN ClinicalTrials.gov number, NCT03148457.)
结论
在本试验中,早期使用DOAC的30天时复发性缺血性卒中、全身性栓塞、颅外大出血、症状性颅内出血或血管性死亡的发生率估计范围为2.8个百分点至0.5个百分点(基于95%置信区间)。(由瑞士国家科学基金会等资助; ELAN ClinicalTrials.gov编号,NCT 03148457。)
编辑丨国康
审核丨杨威 边圆 徐峰
IE-Learning急危重症学习平台
原创声明:文章权限归原作者所有,如需转载请联系我平台。
